 This post is very different than anything I’ve previously written; it’s more philosophical than psychological and is an example of Theoretical and Philosophical Psychology, a small but important niche within psychology that provides critical analyses of the underlying assumptions [philosophies] of psychology and the related sciences. My post is not meant to attack the neurosciences (after all, that is my field of specialization); rather, it is meant to expose the philosophical underpinnings of neuroscience. The alternative assumptions I write about are not necessarily superior, just different. Feel free to contact me with any questions or if you are interested in the references I cite.
This post is very different than anything I’ve previously written; it’s more philosophical than psychological and is an example of Theoretical and Philosophical Psychology, a small but important niche within psychology that provides critical analyses of the underlying assumptions [philosophies] of psychology and the related sciences. My post is not meant to attack the neurosciences (after all, that is my field of specialization); rather, it is meant to expose the philosophical underpinnings of neuroscience. The alternative assumptions I write about are not necessarily superior, just different. Feel free to contact me with any questions or if you are interested in the references I cite.
This post is an exposition of the naturalistic assumptions in the article An fMRI Study of Personality Influences on Brain Reactivity to Emotional Stimuli by Canli et al. (2001). It will also focus on alternative assumptions. I will first explore the assumption of materialism, one half of Descartes’ dualism, and contrast this assumption with a holistic monism. Then I will discuss biological determinism as well as an alternative assumption to it, namely agency.
Materialism accounts for one half of the Cartesian dualism (and thus has been termed a one-sided dualism), the theorized split between mind and matter. It is defined as the notion that “biological explanations will (eventually) be able to fully account for and explain…psychological phenomena” (Hedges, p. 3). Materialism assumes that biology is sufficient to explain behavior. This article is focused on “the neural correlates of emotion [and personality] in healthy people” (p. 33) by using brain imaging techniques. This is an example of materialism in that the authors are looking for “the biological basis [or an objective foundation] of emotion [a subjective phenomenon]” (p. 33). The authors’ assumption of materialism will become clearer with another example. Canli et al. state: “The similarity in the dimensional structure of personality and emotion is due to a common neural substrate where personality traits moderate the processing of emotional stimuli” (p. 33; italics added). What they are saying is that neurons (the brain) are the base and that emotional processing in the brain is affected by personality traits (which they state have a “common neural substrate” with emotions). This is a one-sided dualism—the researchers attempt to explain the subjective experiences of the mind (i.e., emotion) in terms of the material, or biological, body while not including the mind in their methods.
The authors of this study sought to understand emotional responses in terms of neuroimaging. This is an example of method-driven science in that the researchers “ignored…[the] notion of the mind [being immaterial and unpredictable] and focused…on the body” (Slife, p. 13). There is no way to image emotions directly, but by assuming that they are centered in biological reactions, these researchers were able to use traditional scientific methods to measure those reactions. This materialism, or one-sided dualism, has its shortcomings. An alternative way to approach the hypothesis of how personality serves as a “middleman” between the brain and emotions is to use the assumption of a holistic monism. Whereas the authors assume that the brain (body) is the foundation of emotional experience and thus sufficient for that experience, with a monistic assumption the researchers would recognize both body and mind as necessary but not separately sufficient. This would change their study because they would look at a more inclusive picture of people, not just biology and mind but context as well. All of these conditions interact and are only understood in relation to one another. The authors would also consider qualitative measures of life experience and meaning and research those, taking a pluralistic approach.
Another prevalent assumption, which is inseparable from materialism and is in fact a subset of it, is that of biological determinism. Whereas my materialism section focused on the authors’ attempts to explain subjective experiences by their “objective” methods, this one will focus on how they explain varying emotions as caused by variations in biological factors. The authors end their paper on a strong deterministic note: “The different brain activation patterns that these pictures produce…may result in two different subjective interpretations of the identical objective experience” (p. 39). Although they hedge their statement with a may, what they are saying is that their subjects all had the same “objective experience” but because of apparent differences in how their brains responded, this difference caused the variation in subjective emotional interpretation. They imply that people’s interpretations are determined by biology, which rules out agency.
Alternately, when viewing this article according to holistic monism, specifically agency, there are would be many changes in it. First off, it would not be a problem to recognize the role agency plays in the body. The authors would assume that the body affects agency and vice versa–they constitute each other. Instead of “different brain activation patterns” (p. 39) causing different interpretations of emotion it could be that the interpretations affect the neuronal firing instead (or an interplay of both). Also, with an alternative assumption, the following hypothesis would no longer be deterministic: “Extraversion is associated with greater brain reactivity to positive” (p. 34). The authors imply that personality traits are biologically based (see paragraph 2 of this paper)–even if behaviorally influenced; therefore, biology causes personality which causes changes in brain reaction (which are experienced subjectively by people as emotions). Alternatively, this can be explained by “agentic factors” (Slife, p. 25), such as people choosing (even unconsciously) how to respond to the pictures. Also, instead of personality being determined by the brain, manifestations of agency (choices) in a context (e.g., experiences) could shape personality.

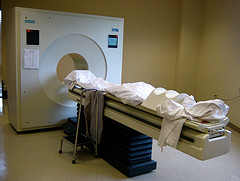 The positron emission tomography (PET) scan measures blood flow in the brain. This is accomplished by injecting a person or animal with a radioactive isotope (i.e. an unstable atom, usually a variation of oxygen that has a short-half life); this isotope will quickly decay. Founded on the assumption that blood flow will increase in areas of the brain that are in heavy use (such as when a person is viewing an object or reading words or some other cognitive-intensive function), a fair portion of the injected isotopes will end up in the active part of the brain. As the isotopes decay, a positron (a small particle with the exact opposite charge as an electron) is released. This positron will collide with an electron and they will annihilate each other, sending two gamma ray particles in exactly opposite directions. These gamma rays are picked up by the PET scanner, which then determines where they came from in the brain. Since blood should concentrate where the brain is activated, there should be higher levels of isotopes there and this will show up on the scanner in the form of increased levels of gamma rays. The test is usually run twice (once as the control condition and once as the experimental). The difference between the two conditions is measured and any difference should show what area(s) of the brain was (or were) activated.
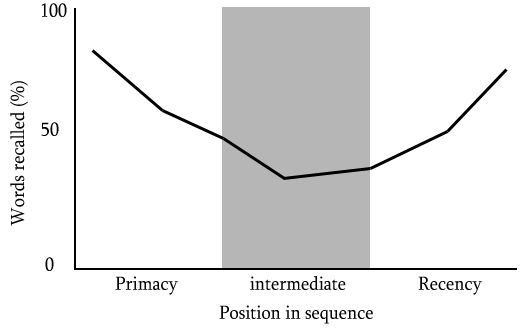
The positron emission tomography (PET) scan measures blood flow in the brain. This is accomplished by injecting a person or animal with a radioactive isotope (i.e. an unstable atom, usually a variation of oxygen that has a short-half life); this isotope will quickly decay. Founded on the assumption that blood flow will increase in areas of the brain that are in heavy use (such as when a person is viewing an object or reading words or some other cognitive-intensive function), a fair portion of the injected isotopes will end up in the active part of the brain. As the isotopes decay, a positron (a small particle with the exact opposite charge as an electron) is released. This positron will collide with an electron and they will annihilate each other, sending two gamma ray particles in exactly opposite directions. These gamma rays are picked up by the PET scanner, which then determines where they came from in the brain. Since blood should concentrate where the brain is activated, there should be higher levels of isotopes there and this will show up on the scanner in the form of increased levels of gamma rays. The test is usually run twice (once as the control condition and once as the experimental). The difference between the two conditions is measured and any difference should show what area(s) of the brain was (or were) activated. One experiment about cognitive brain functioning is the word superiority effect findings of Dr. Reicher in 1969. In this experiment either a word or a non-word (string of letters) is flashed on a screen. The subject is asked if the stimulus contained one of two letters, say a “C” or an “E”. When the stimulus did not resemble a word (e.g., XXCX) subjects were correct in identifying the target letter about 80% of the time. When the string of letters was similar to a word but not one (e.g., FELV) the subjects also correctly identified the target letter 80% of the time. However, the interesting finding was that when the stimulus was a word (e.g., TEND), subjects were correct in identification 90% of the time. So the word superiority effect is that subjects are most accurate in identifying a target letter when it is contained in a word as opposed to a string of letters.
One experiment about cognitive brain functioning is the word superiority effect findings of Dr. Reicher in 1969. In this experiment either a word or a non-word (string of letters) is flashed on a screen. The subject is asked if the stimulus contained one of two letters, say a “C” or an “E”. When the stimulus did not resemble a word (e.g., XXCX) subjects were correct in identifying the target letter about 80% of the time. When the string of letters was similar to a word but not one (e.g., FELV) the subjects also correctly identified the target letter 80% of the time. However, the interesting finding was that when the stimulus was a word (e.g., TEND), subjects were correct in identification 90% of the time. So the word superiority effect is that subjects are most accurate in identifying a target letter when it is contained in a word as opposed to a string of letters.
